
Dialectical Behavior Therapy: A Definitive Guide
Last updated: March 2026
Dialectical Behavior Therapy
A Definitive Guide
This is the ultimate guide to understanding Dialectical Behavior Therapy (DBT). The primary goal of this article is to assist those who are experiencing emotional, relationship, or behavioral issues in their lives.
So if you want to:
- Improve your behavior
- Build your personality
- Improve Quality of Life
- Want to get a deeper understanding of DPT
- Improve Mental Health
- Want to have a diverse knowledge of different therapies along with uses

And many more, then you will love this guide.
Let’s get started!
Contents

Chapter 1
Basics of DBT

Chapter 2
Strength of DBT

Chapter 3
DBT strategies

Chapter 4
DBT v/s CBT

Chapter 5
Core Benefits of DBT

Chapter 6
Steps in DBT that can boost your self-esteem

Chapter 7
Tips to Become a Successful DBT Therapist
Chapter 1:
Basics of DBT
This is the first introductory chapter of DBT which consists of the basics of Dialectical Behavior Therapy. In this chapter, you will look at the definition of DBT along with the terms “D” and “B” in DBT. You will also look at the historical background of DBT. How did this start?
What is the origin of DBT along with the transformation of DBT from the early days to the modern era?


Definition of DBT
DBT is intended to help people who have seen little or no improvement with other types of therapy.
This therapy emphasizes problem-solving and acceptance-based strategies. It operates within the context of dialectical methods. DBT is effective in treating a variety of other disorders, including substance abuse, depression, post-traumatic stress disorder (PTSD), and eating disorders.
DBT is thus a trans-diagnostic, modular treatment. DBT is part of the "third wave" of cognitive-behavioral therapy, and it extends CBT to help patients manage stress. In the therapy of psychological difficulties, DBT aims to have the patient see the therapist as an ally rather than an opponent.
As a result, the therapist strives to embrace and validate the client's feelings at any given time while also informing and offering the client better alternatives to certain sentiments and behaviors. DBT focuses on the client learning new skills and altering their behaviors in order to achieve a "life worth living," as defined by the patient.
Clients have a biological propensity for emotional dysregulation, and their social context validates maladaptive behavior, according to DBT's biosocial theory of BPD. In some therapeutic settings, DBT skills training alone is being used to address treatment goals, while DBT's broader purpose of emotion regulation has allowed it to be applied in new settings, such as assisting parenting. To sum it up:
“DBT is an abbreviation for dialectical behavior therapy. It's a type of therapy that can teach you how to deal with difficult emotions. It is an all-encompassing cognitive behavioral treatment. Suicidal and other self-destructive behaviors may be treated with DBT. It teaches patients how to cope with and change harmful behaviors.”
What is Dialectical or “D’ in DBT?
The letter "D" in DBT stands for "dialectical." A dialectic is an integration or synthesis of opposites. Dialectical methods are used in DBT to help both the therapist and the client get out of extreme positions. The term "dialectical" refers to the belief that combining two opposites in treatment, acceptance, and transformation, yields better results than either one alone. The ability to analyze matters from different viewpoints and arrive at the most economical and acceptable reconciliation of seemingly contradicting facts and stances is what dialectical thinking refers to.
What is “B” in DBT?
The letter “B” in DBT is Behavioral. Individuals, organisms, systems, and artificial entities engage in a variety of acts and mannerisms as part of their behavior. Other systems or species, as well as the inanimate physical environment, can be included in these systems. A behavioral approach is required for DBT. This means that we evaluate events and target behaviors that are relevant to the clients' objectives in order to find out how to address their difficulties.
What is the origin of DBT?
DBT's efficacy has been supported by a significant body of research spanning decades. This form of treatment is now used in dozens of countries throughout the world. When it comes to DBT's beginnings, you'll want to know when it began and who initiated it.
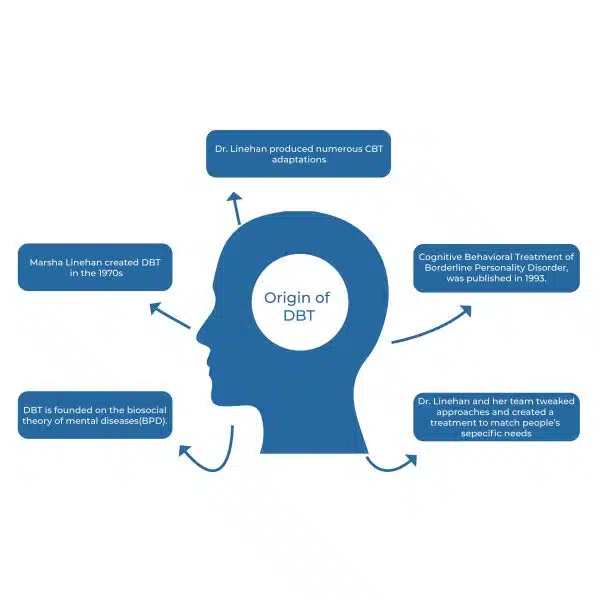
Who first started the DBT?
Marsha Linehan created DBT in the 1970s. DBT was developed as a result of her work with two mental health populations: those with suicidal ideation and people with a borderline personality disorder.
The growing popularity of Cognitive Behavioral Therapy piqued Linehan's interest (CBT). In her practice, she chose to use standard CBT. After performing research on the effectiveness of CBT in her target demographic, Linehan and her colleagues ran into problems. They observed three key issues with the use of traditional CBT:
- The change-focused interventions were perceived as invalidating by the participants. Withdrawal from therapy, animosity toward therapists, and a mix of both were common reactions to these feelings.
- Participants and therapists reenacted a reinforcement cycle in which positive effort was stopped, and avoidance and redirection were rewarded. Participants became enraged when therapists pushed for change. Participants responded with warmth and positive feedback when therapists allowed a subject change. This loop appeared to deceive both the therapist and the participant into believing they were on the correct track when they were not.
- Because of the sensitivity of crisis circumstances, therapists spent a significant amount of time addressing safety concerns, such as suicidal thoughts or gestures, animosity, and threats directed towards the therapist, or self-injurious behaviour. There was frequently insufficient time to teach coping techniques or handle behavioral issues.
Linehan produced numerous CBT adaptations after evaluating these issues. These immediately addressed the population's needs. Before participants were instructed to focus on change, acceptance-based strategies were used to ensure that they felt supported and validated.
Dialectics were also used to assist therapists and treatment participants to concentrate on the synthesis of polar opposites like acceptance and change. This allowed them to avoid becoming caught in severe position-taking habits.
CBT was modified to include these and other modifications. Linehan's first formal treatment manual, Cognitive Behavioral Treatment of Borderline Personality Disorder, was published in 1993. Since then, DBT has become increasingly popular.
When was DBT started?
Dr. Marsha Linehan and colleagues officially started DBT in the late 1980s after discovering that cognitive-behavioral therapy (CBT) alone did not function as well as expected in individuals with BPD. Dr. Linehan and her team tweaked approaches and created a treatment to match these people's specific needs.
Transformation of DBT from Early Days to Modern Era
DBT has evolved into a process in which the therapist and client work together to balance and synthesize acceptance and change-oriented tactics, similar to the philosophical dialectical process of thesis and antithesis, followed by synthesis. DBT emerged from a succession of failed attempts in the late 1970s to apply normal Cognitive Behavioral Therapy (CBT) techniques to chronically suicidal individuals. DBT has been used to treat persons with depression, drug and alcohol problems, post-traumaticc stress disorder (PTSD), traumatic brain injuries (TBI), binge-eating disorder, and mood disorders, according to research.
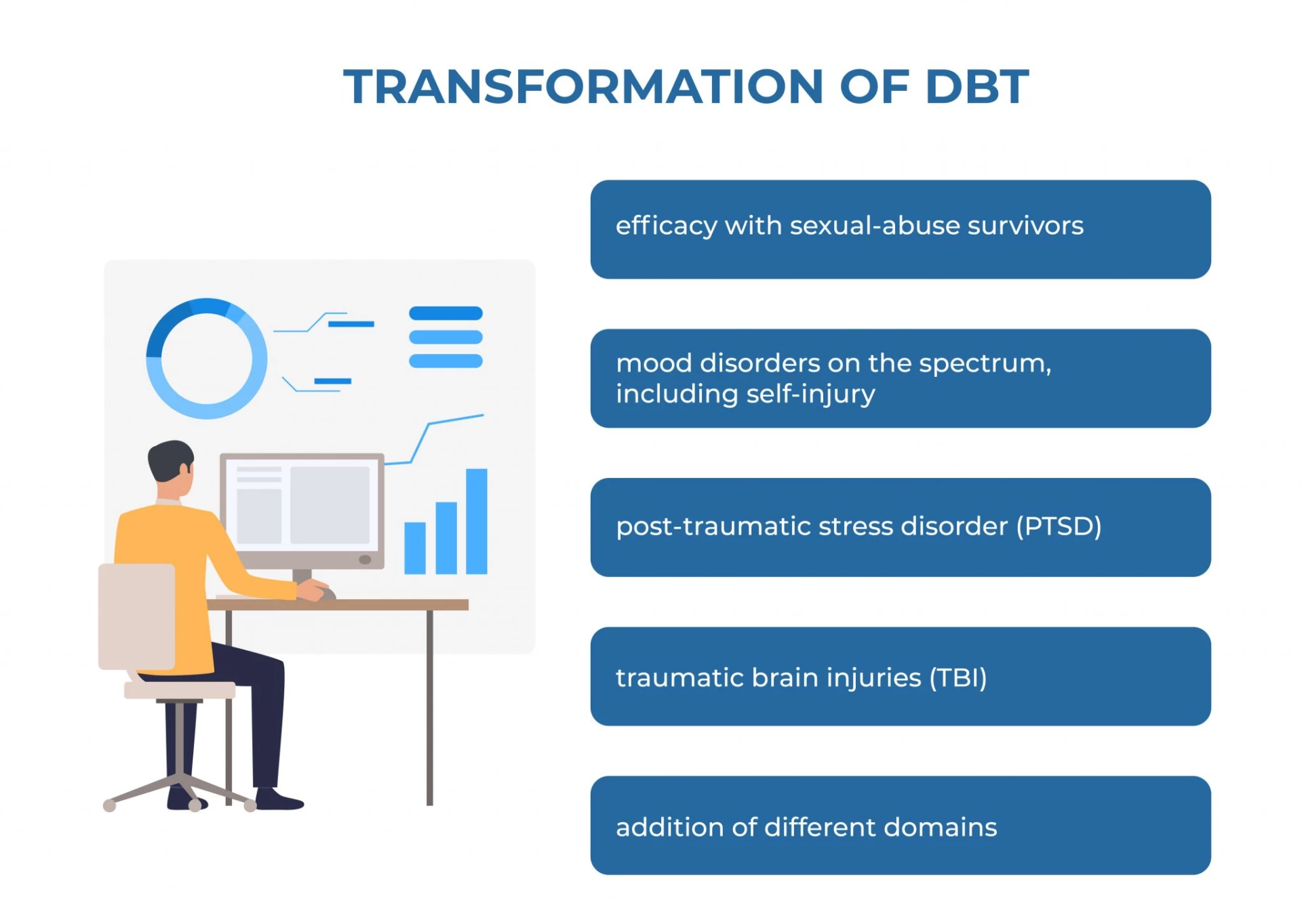
In the modern era, DBT appears to help individuals with symptoms and behaviors linked with mood disorders on the spectrum, including self-injury, according to research.
Its efficacy with sexual-abuse survivors and chemical dependency has also been demonstrated in recent research. Over time, DPT has added different domains to it. Today, it is not only confined to emotional behavior.
DBT integrates normal cognitive-behavioral strategies for emotion regulation and reality checking with contemplative meditation principles of distress tolerance, acceptance, and awareness.
DBT is the first therapy to be empirically proved to be usually helpful in treating borderline personality disorder. It is founded on the Biosocial Theory of Mental Disease (BPD).
Compared to standard treatment, the first randomized clinical trial of DBT demonstrated a lower incidence of suicide gestures, psychiatric hospitalizations, and treatment drop-outs. DBT had moderate effects in people with high blood pressure, according to a meta-analysis. So, DBT has extended domains in the modern era. As you are now aware of DBT's origins, the next chapter will focus on the strengths of DBT.
Chapter 2:
Strengths of DBT
In this chapter, you will look at the major strengths of DBT. Basically, this chapter aims to see the treatment which is covered by DBT. Dialectical behavior therapy covers a wide range of emotional disturbances including stress, suicidal thoughts, behavior problems, etc. DBT is an effective treatment for these issues.
I'll lead you through the stages of DBT treatment and the goals you should set for yourself.

What does DBT treat?

Self-harming Treatment:
Self-injury, often known as self-harm, refers to any intentional, self-inflicted harm that is not intended to be suicidal.
Anyone who has had personal experience with the condition, whether it is from oneself or a loved one, realizes how terrible and severe it can be. Those who have no experience with self-harm frequently make incorrect assumptions about those who do it.
Increased awareness leads to a stronger feeling of understanding and empathy, which is why Self-Injury Awareness Day is so important. It alleviates the shame and stigma associated with self-injury, hopefully encouraging people to seek help.
Self-injury sufferers can feel alienated and alone, cut off from friends, family, and loved ones. Self-harm provides emotional release or a sense of control over one's life.
However, that feeling of relaxation and control is only fleeting, and it usually leads to a vicious cycle. Many people are hesitant to seek help for self-harm because they are unsure whether it will be effective.
If you're trying to overcome your self-injury issues, help and solutions are available. Dialectical Behavior Therapy, for example, provides four behavior skills that are useful for learning to quit self-harming behaviors. Self-harm treatment is, thankfully, available. When it comes to resolving self-injury behaviors, talk therapy is the most common treatment option. The patient, in consultation with their counselor or psychiatrist, examines and addresses the immediate motivations for these actions.
Then they investigate and address the fundamental causes of their self-harm. One of the most effective approaches for working with these people is Dialectical Behavior Therapy (DBT). It was created to help those with prolonged suicidal ideation, especially those who had a borderline personality disorder.
DBT is a type of solution-focused treatment that focuses on identifying and replacing problematic behaviors with good ones.
Mindfulness, distress tolerance, interpersonal effectiveness, and emotional regulation are the four core skills employed in DBT. All four are necessary tools for overcoming self-injury and building more effective coping mechanisms. The details of each will be studied in the following chapters.
Depression Treatment:
DBT has been shown to be useful in the treatment of a variety of emotional and behavioral issues, including depression. When you're dealing with severe feelings of emotional sorrow, getting through the symptoms of depression might be difficult. DBT can help you accept yourself and your current position more readily, allowing you to be more motivated to make changes.
The following are some of the symptoms of depression that may improve with DBT:
- Lack of enthusiasm for previously enjoyed activities
- Sadness that persists
- Focusing, concentrating, or remembering problems
- Body aches and pains, as well as headaches, are physical indications of depression.
DBT can assist you in managing uncomfortable emotions and developing effective coping skills in the face of adversity. You'll try to strike a balance between acceptance and transformation with the support of your therapist. You'll gradually be able to improve negative or unhealthy ideas, resulting in less or less severe depressive symptoms.
DBT may be the solution you're looking for if other treatment approaches aren't producing the results you want. You may experience depression if you are plagued by chronic, crushing feelings of despair or hopelessness.
Positive feedback from your therapist or support group, together with the acquisition of new life skills, can help you feel more driven to change and work toward a life worth living with DBT.
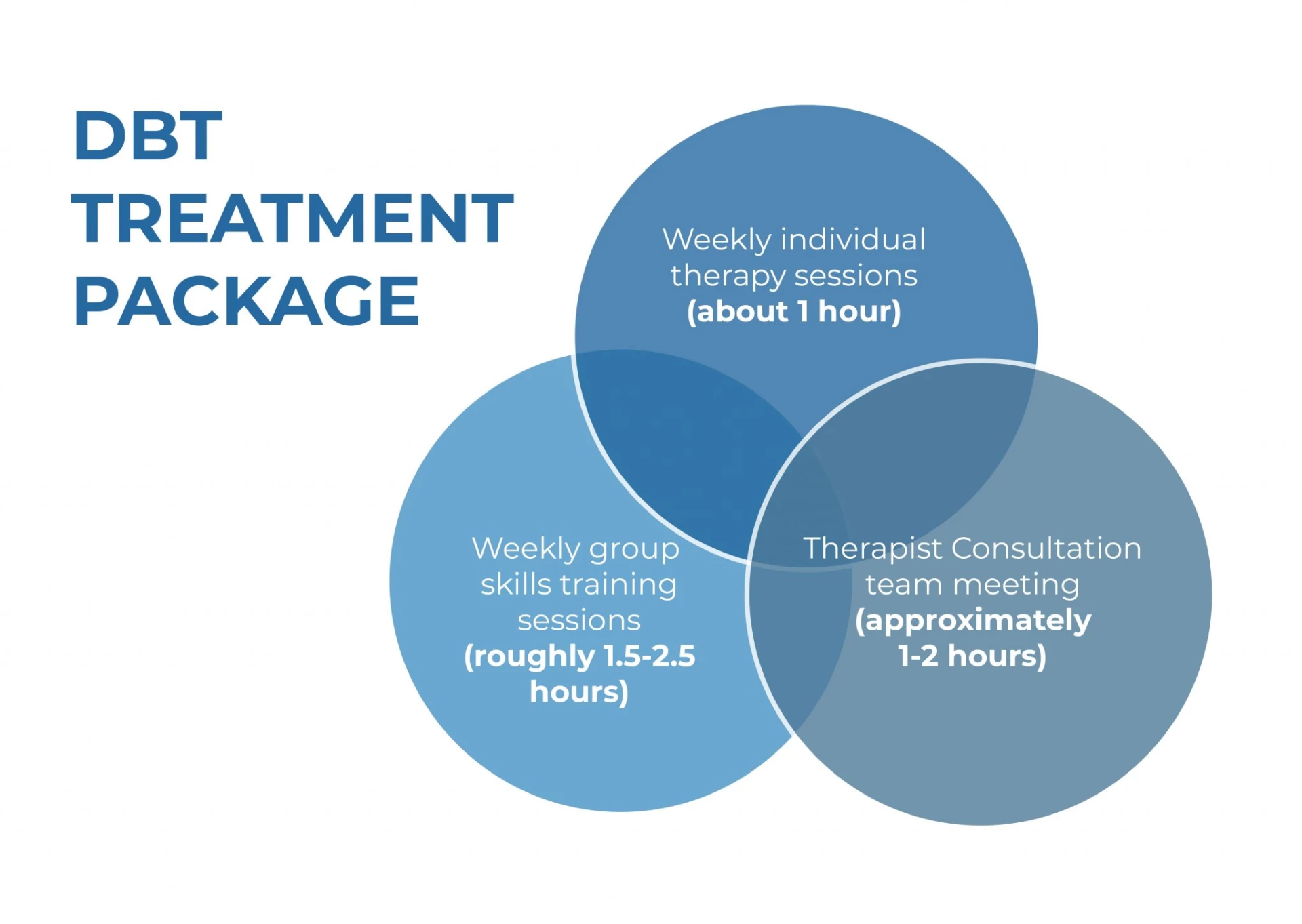
Weekly individual therapy sessions (about 1 hour), weekly group skills training sessions (roughly 1.5–2.5 hours), and a therapist consultation team meeting (approximately 1–2 hours) make up the typical DBT treatment package.
Suicide Attempts Treatment:
Dialectical Behavioral Therapy has been the most successful treatment for patients with suicidal and self-harming behaviors for decades.
DBT is one of the few treatments that has been shown to be beneficial in reducing suicidal ideation and behavior. The goal is to help people find deep-seated meaning and purpose in order to keep them alive and well in the long run, not merely to prevent suicide or self-harm.
Unlike therapies that aim to lower suicide risk indirectly by addressing underlying problems, DBT directly addresses suicidal thoughts and behaviors as the primary issue to be addressed. This entails determining the variables that are driving or maintaining specific episodes of suicidal thoughts and behaviors, as well as developing ways to address these issues.
At the start of each therapy session, DBT therapists ask clients to rate their present inclinations to kill themselves. This type of regular monitoring is necessary for therapists to respond when suicidal desires are severe, as well as to examine the elements that cause rises and declines in suicidal urges over time.
DBT strives to treat high-risk clients in the least restrictive environment feasible. When the danger of suicide is high, DBT therapists do not often recommend or rely on psychiatric hospitalization.
This strategy is based on a lack of evidence that mental hospitalization reduces suicide risk, as well as concerns that it may raise long-term danger. Furthermore, the DBT paradigm implies that people cannot have a normal quality of life if they are in and out of psychiatric hospitals on a regular basis and that clients must learn how to lower suicide risk while remaining in their natural living circumstances.
DBT helps people avoid costly crisis treatments like psychiatric hospitalizations and emergency department visits while also reducing suicidal behavior.
Eating Disorder Treatment:
DBT is based on the assumption that our incapacity to appropriately manage our emotions is the root of most mental health issues.
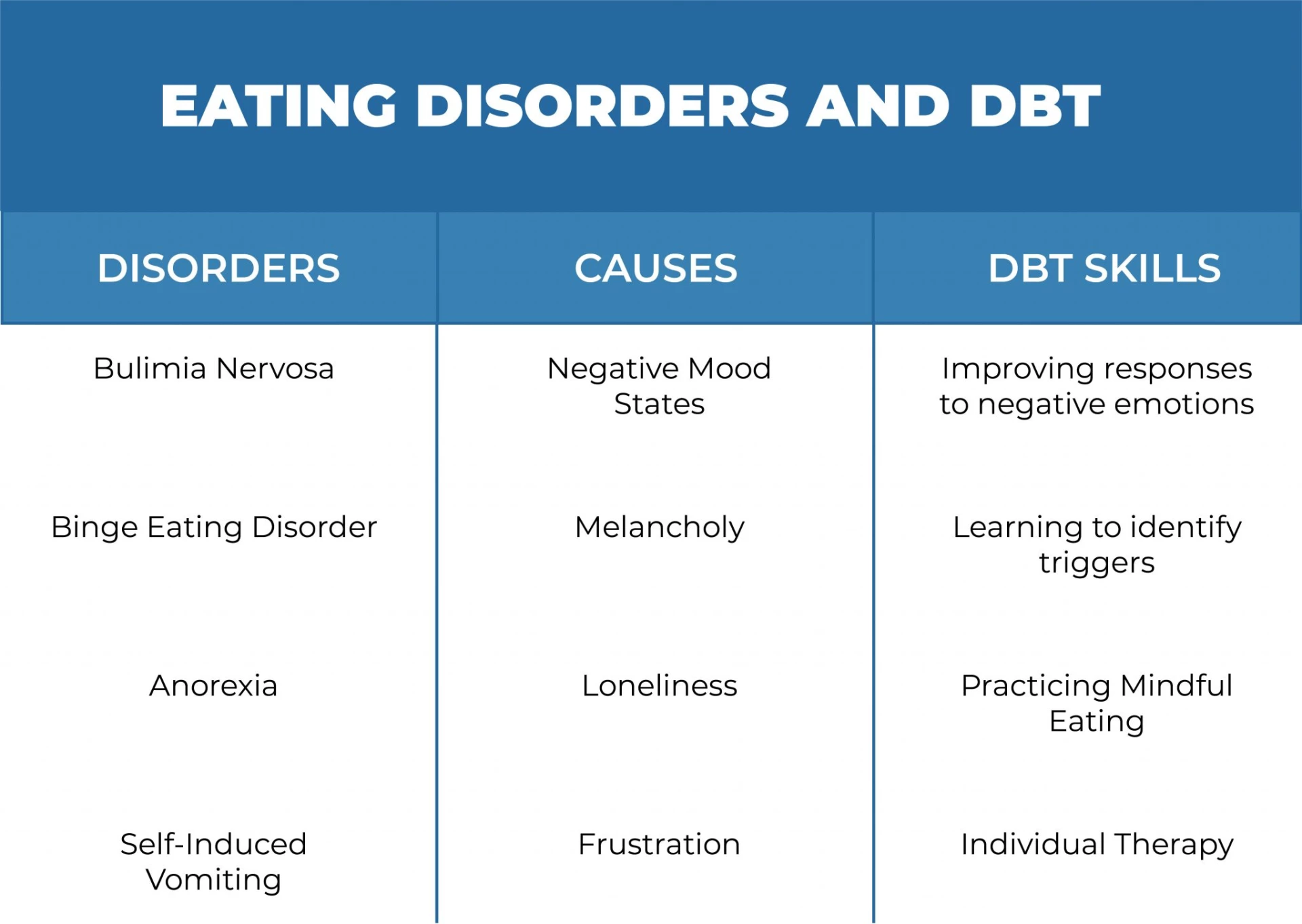
Eating disorders, particularly binge eating and purging, are well-suited to this concept. We know that negative mood states like melancholy, loneliness, frustration and rage can trigger eating disorder behaviors like binge eating and purging.
This is because these feelings are unpleasant to experience. Thus people want to avoid or escape them as much as possible. This can be found in binge eating and purging behaviors. As a result, DBT aims to teach people how to use better-coping methods. It's vital to note that DBT is only used to treat bulimia nervosa and binge eating disorder, not anorexia nervosa.
Individual therapy and skills training are used in an adapted version of DBT developed specifically for the treatment of eating disorders. DBT techniques can be taught and incorporated into different treatment approaches on their own. DBT skills are useful not only for people with eating disorders but for anybody trying to enhance their quality of life.
What are the stages and targets of DBT treatment?
There are targets for each stage that are prioritized based on their relevance to the patient's daily behavior and the session at hand.
As a result, in individual treatment, this is a goal-oriented agenda. Individual and group goals varied, as did intersession communication methods such as texting, emailing, or contacting the patient. Each of these has various goals.
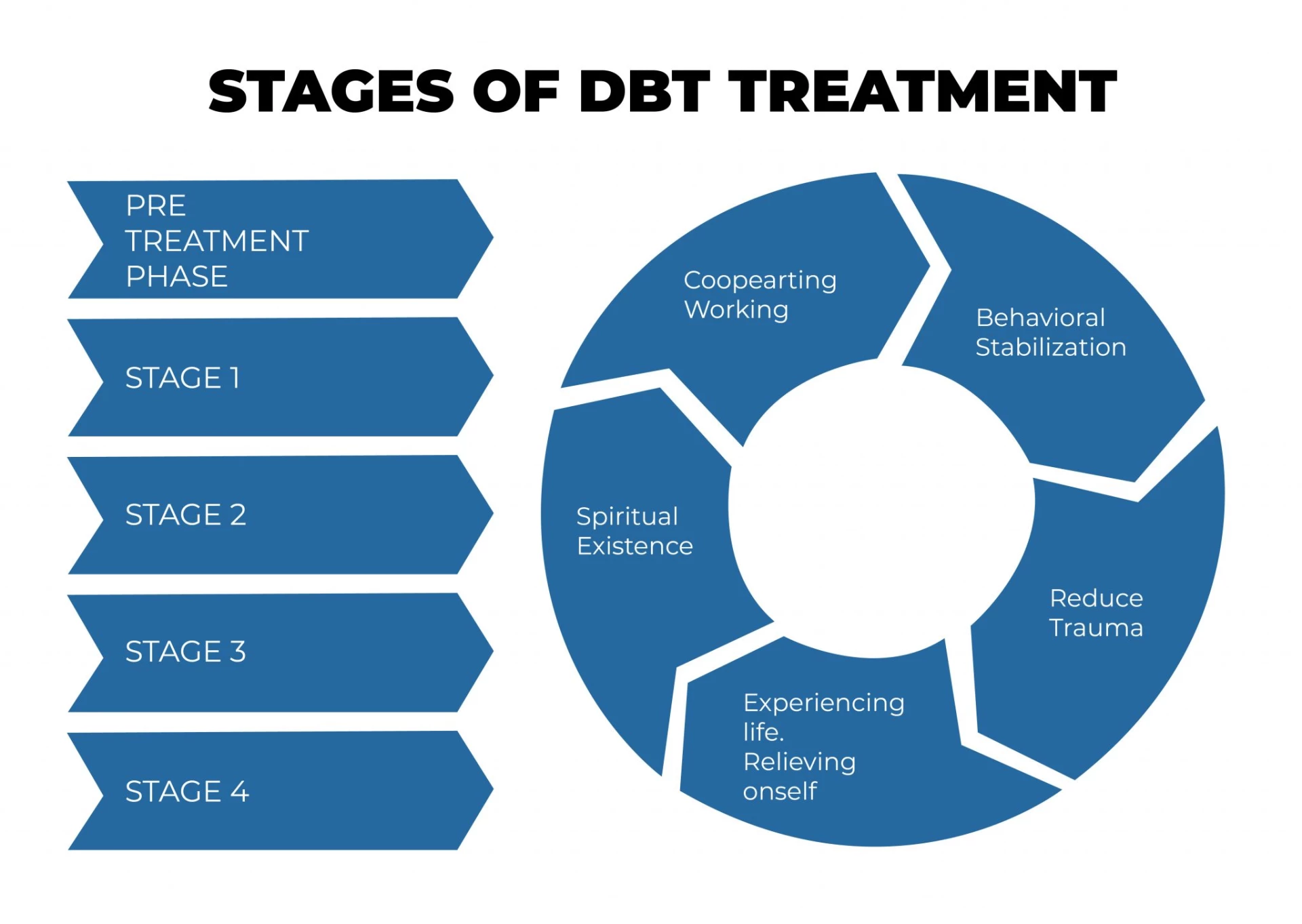
So let’s discuss each phase.
Pre-Treatment Phase:
DBT treatment is divided into four stages and goals. The pre-treatment phase, which every potential DBT client is required to complete, is not included in the four stages and targets. The therapist and client often join stage 1 after getting through the pre-treatment phase and determining that they can work together.
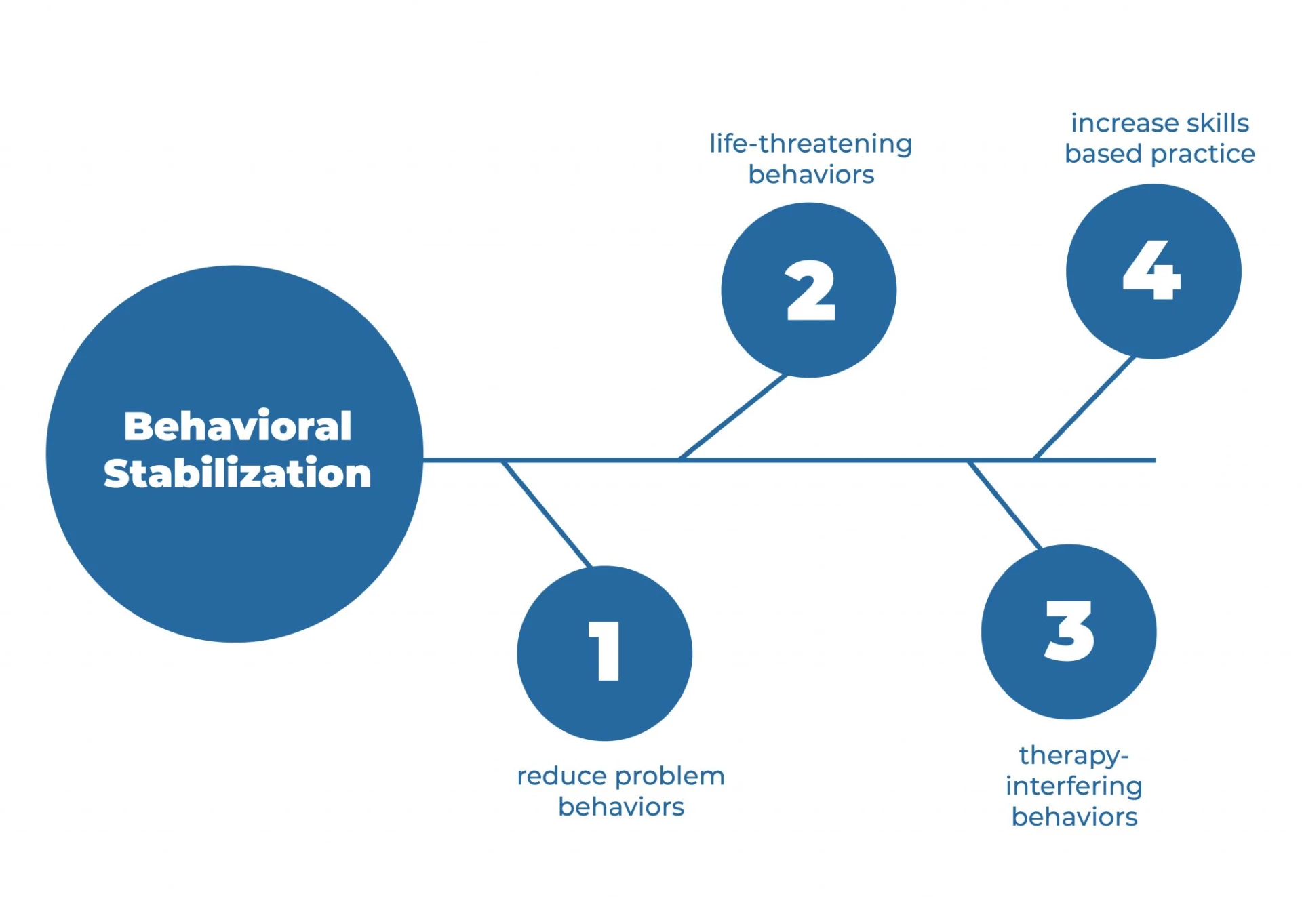
Stage 1: Behavioral Stabilization:
Stage 1 is when the therapist and client collaborate to reduce problem behaviors, life-threatening behaviors, therapy-interfering behaviors, and increase skills-based practice.
In stage 1, the patient will be learning skills. It's critical to note that the stages are not in any particular order. They're truly circular, which means that specific difficulties in each stage may need to be revisited by the therapist and the client.
As a result, it is very uncommon for a patient to complete stage 1, move on to stage 2, and then return to stage 1.
Stage 2: Reduce Trauma:
Stage 2 entails minimizing any trauma-related symptoms, such as formal diagnoses of Posttraumatic Stress Disorder (PTSD) and other painful emotional events that may or may not meet the criteria for PTSD.
Additionally, invalidating emotional events that clients may have had as children can be discussed here. It is critical not to increase the heat in therapy until you are in stage 2. Because we're processing traumatic histories and amplifying emotion, stage 2 is turning up the heat. It's critical to avoid exacerbating the patient's already distressing emotional experiences from stage 1.
It's unrealistic to expect a patient to completely resolve all stage 1 behavior before going on to stage 2. The most crucial thing to control is suicidal and self-harming behaviors. Before advancing into stage 2, DBT therapists would propose a certain period of time for a patient to abstain from life-threatening conduct.
Before moving on to stage 2, patients must make a commitment to refrain from life-threatening behavior. When it comes to therapy-interfering or quality-of-life-interfering conduct, the therapist should think about the intensity and frequency of both.
By the time a client reaches stage 2, they should have a solid understanding of the abilities taught in group skills training.
Stage 3 and 4:
Stages 3 and 4 in DBT theory are not as evolved as stages 1 and 2. In reality, little is known about stage 3, which entails experiencing life, believing in oneself, and achieving personal goals, or stage 4, in which the patient finds greater significance through a spiritual existence.
The majority of DBT research that has been studied has focused on stages 1 and 2. Important points Four stages plus a pre-treatment phase are included in standard DBT. Pre-treatment is required for all patients. There is no set order in which these stages must be completed.
Each stage has its own set of goals. The majority of patients start in stage 1. The first stage, which involves behavioral stabilization, is the most commonly mentioned. The patient should continue in stage 1 if they have life-threatening behaviors, self-harm, or major therapy-interfering or quality-of-life interfering behavior. Stage 2 does not address childhood history or trauma histories. Finally, there is relatively little information about treatment for phases 3 and 4. After looking at the strengths of DBT, I'll take you to the next chapter, where you'll learn about DBT's strategies.
Chapter 3:
DBT strategies
This chapter aims at the basic 4 modules of DBT that are mindfulness, acceptance and change, distress tolerance, and emotional regulation. In both individual and group treatment, skill development in these four modules is traditionally done in a systematic and gradual manner. So you must understand the specifics of these modules and how they function.
So, let’s start this interesting chapter in depth.

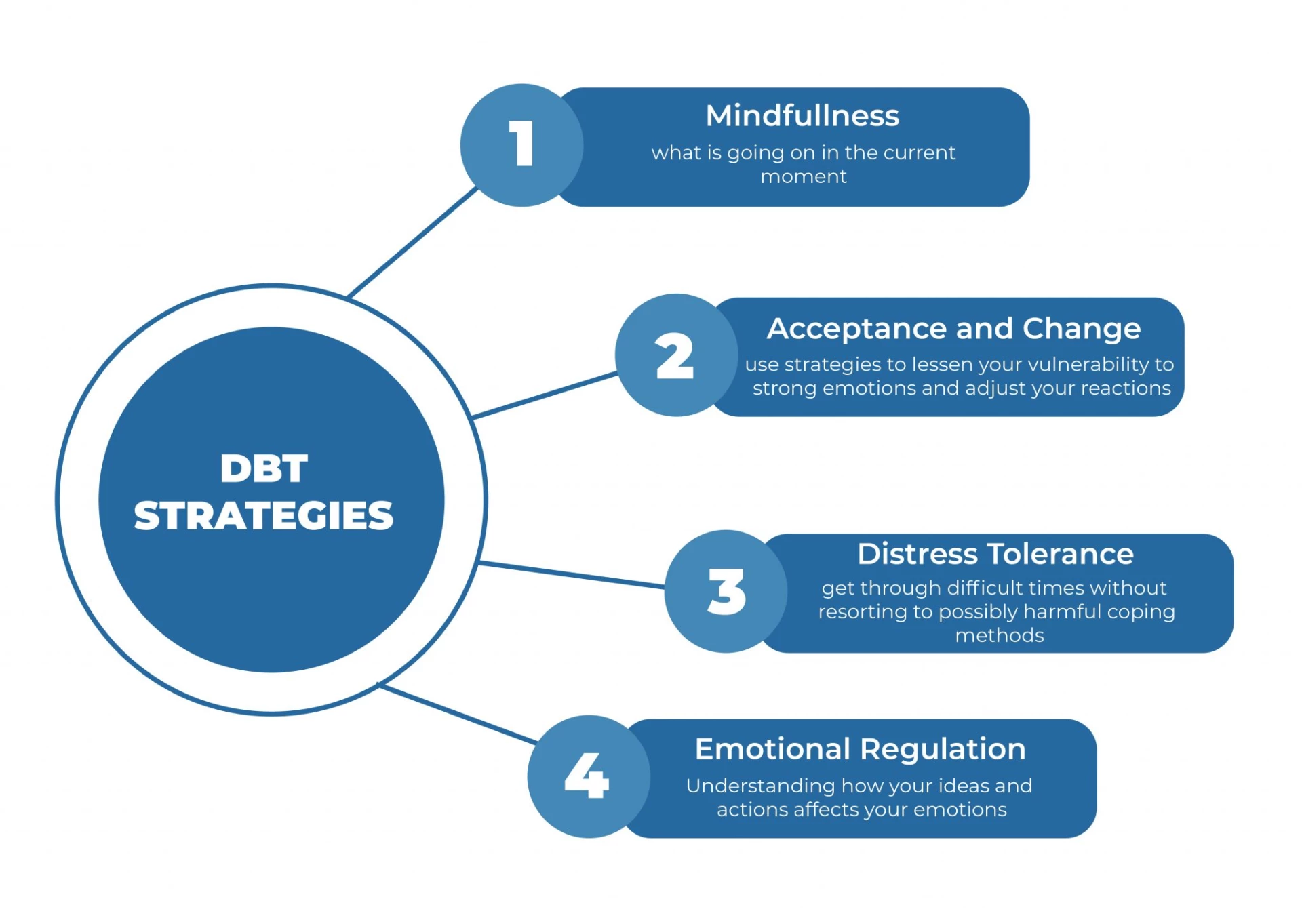
Mindfulness
Being mind-full means being aware of and embracing what is going on in the current moment. This can assist you in learning to observe and accept your thoughts and feelings without condemnation.
All parts of DBT are built around the concept of mindfulness. Because it helps people accept and tolerate the overwhelming feelings they may experience when questioning their behaviors or exposing themselves to stressful events, it is considered a foundation for the other DBT skills. Mindfulness and the meditation activities used to teach it are based on traditional contemplative religious practice, albeit the DBT version does not include any religious or metaphysical beliefs.
It is the skill to pay attention to the current moment without judgment. It is about living in the now, completely experiencing one's emotions and senses while maintaining perspective.
Mindfulness can also be used to increase awareness of one's surroundings through the five senses of touch, smell, sight, taste, and sound. The notion of acceptance, often known as "radical acceptance," is central to mindfulness. Acceptance skills rely on the patient's ability to look at things objectively and accept situations and their feelings.
This reduces overall distress, which can lead to less discomfort and symptomatology. This ability, like mindfulness-based therapy, allows you to live in the present moment and accept what is happening right now.
We have a tendency to live in the future when we are anxious, trying to foresee what will happen in every event. The difficulty with this is that no one can anticipate the future, thus it will always be a mystery to some degree.
In contrast, when we are depressed, we tend to get caught in the past and reflect on what could have or should have been. The inability to modify the past or go across time is the issue here.
The following are some DBT mindfulness skills:
- Concentrate more on the present moment.
- Without passing a verdict, observe your thoughts, emotions, and bodily sensations.
- Exercises in mindful breathing that can bring you into the present moment.
- During attentive meditation, be nice and sympathetic to oneself.
Acceptance and Change
The argument of acceptance and change is introduced in the first few sessions of DBT. DBT strategies can flourish if the patient and therapist have built a trusting relationship.
Understanding radical acceptance is an important component of understanding acceptance: radical acceptance embraces the idea of facing experiences, both positive and negative, without a verdict. Mindfulness and emotional management skills, which are based on the concept of radical acceptance, are also included in acceptance.
These abilities are what distinguish DBT from other therapies. As it relates to dialectical behavior therapy, dialectics refers to the therapist's role in assisting the patient in resolving some of the conflicts that occur both inside themselves and in the therapeutic interaction throughout therapy.
When compared to community therapy by non-behavioral experts, DBT reduced suicide attempts by 50% and psychiatric hospitalizations for suicidality by 73 percent, according to the data.

You'll learn how to use strategies to lessen your vulnerability to strong emotions and adjust your reactions to acceptance and change.
Issues can be clarified using acceptance and change abilities. These abilities integrate listening, social, and assertiveness training to teach you how to change situations while staying loyal to your ideals.
Among these abilities are:
- Interpersonal effectiveness, or learning how to work through disagreement and obstacles in relationships.
- Objective effectiveness, or learning how to ask for what you want and take action to get it.
- Self-respect effectiveness, or increasing your self-esteem.
Distress Tolerance
Although mindfulness can help, it isn't always enough, especially in times of crisis. Distress tolerance comes into play here.
Distress tolerance skills allow you to get through difficult times without resorting to possibly harmful coping methods. You might employ various coping skills to assist you to deal with your emotions during a crisis.
Some of these, such as self-isolation or avoidance, are ineffective, but they may make you feel better temporarily. Others, such as self-harm, substance abuse, or furious outbursts, may be harmful.
Many current mental health treatment approaches focus on modifying upsetting events and circumstances, such as dealing with a loved one's death, job loss, major illness, terrorist attacks, and other traumatic occurrences. Accepting, making sense of, and tolerating distress have received little attention.
Person-centered, psychodynamic, psychoanalytic, gestalt, or narrative therapies, as well as religious and spiritual communities and leaders, have traditionally taken on this duty. Dialectical behavior therapy stresses effective pain management. Distractions, improving the present, self-soothing, and exercising acceptance of what is are all examples of unhealthy coping habits covered in this module.
DBT mindfulness skills lead to the development of distress tolerance skills.
They have to do with one's ability to accept oneself and the current environment without being critical or judgmental. Because this is a nonjudgmental posture, it does not imply approval or resignation.
Instead of becoming overwhelmed or hiding from unfavorable situations, the goal is to become capable of calmly identifying them and their impact.
This enables people to make informed judgments about whether and how to act rather than succumbing to the powerful, frantic, and often harmful emotional reactions associated with a borderline personality disorder. It prevents you from acting rashly when you're angry or turning to narcotics to relieve your distress.
Emotion Regulation
Emotion Regulation is a Dialectical Behavior Therapy (DBT) ability that helps us comprehend the role of emotions, the action drive that goes along with each emotion, and whether we should obey or resist these urges.
When someone has a history of trauma or feels threatened or abandoned, they may experience emotional extremes they can't control. Emotional dysregulation is the term for it.
They might become excessively reactive and self-destructive when they are triggered or emotionally overloaded. Researchers have discovered that patients with emotional dysregulation may have problems with the neurocircuitry in the brain that governs emotion using Magnetic Resonance Imaging (MRI).
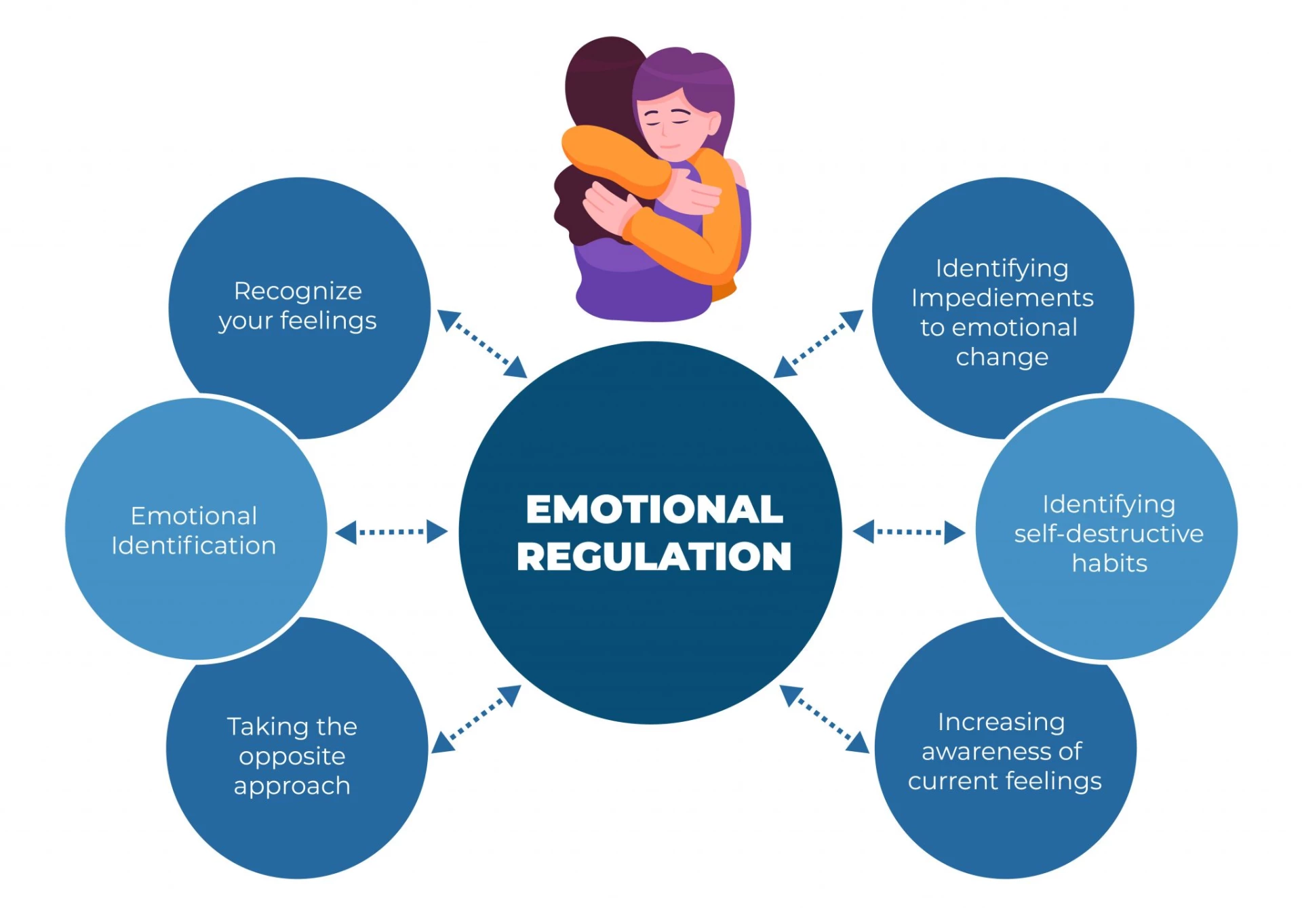
Emotion regulation skills in dialectical behavioral therapy include:
- Recognize your feelings
- Understanding how your ideas and actions affect your emotions
- Identifying self-destructive habits
- Boosting pleasant feelings
- Emotion identification and labeling
- Identifying impediments to emotional change
- Using "emotion mind" to reduce vulnerability
- Enhancing good emotional experiences
- Increasing awareness of current feelings
- Taking the opposite approach
- Using strategies for distress tolerance
Emotional regulation abilities are founded on the premise that powerful emotions are a conditioned response to distressing experiences, the conditioned stimulus, and that they are necessary to change the patient's conditioned response.
Understanding and labeling emotions, changing undesired feelings, lowering susceptibility, and managing harsh conditions are the four modules that these talents fall within.
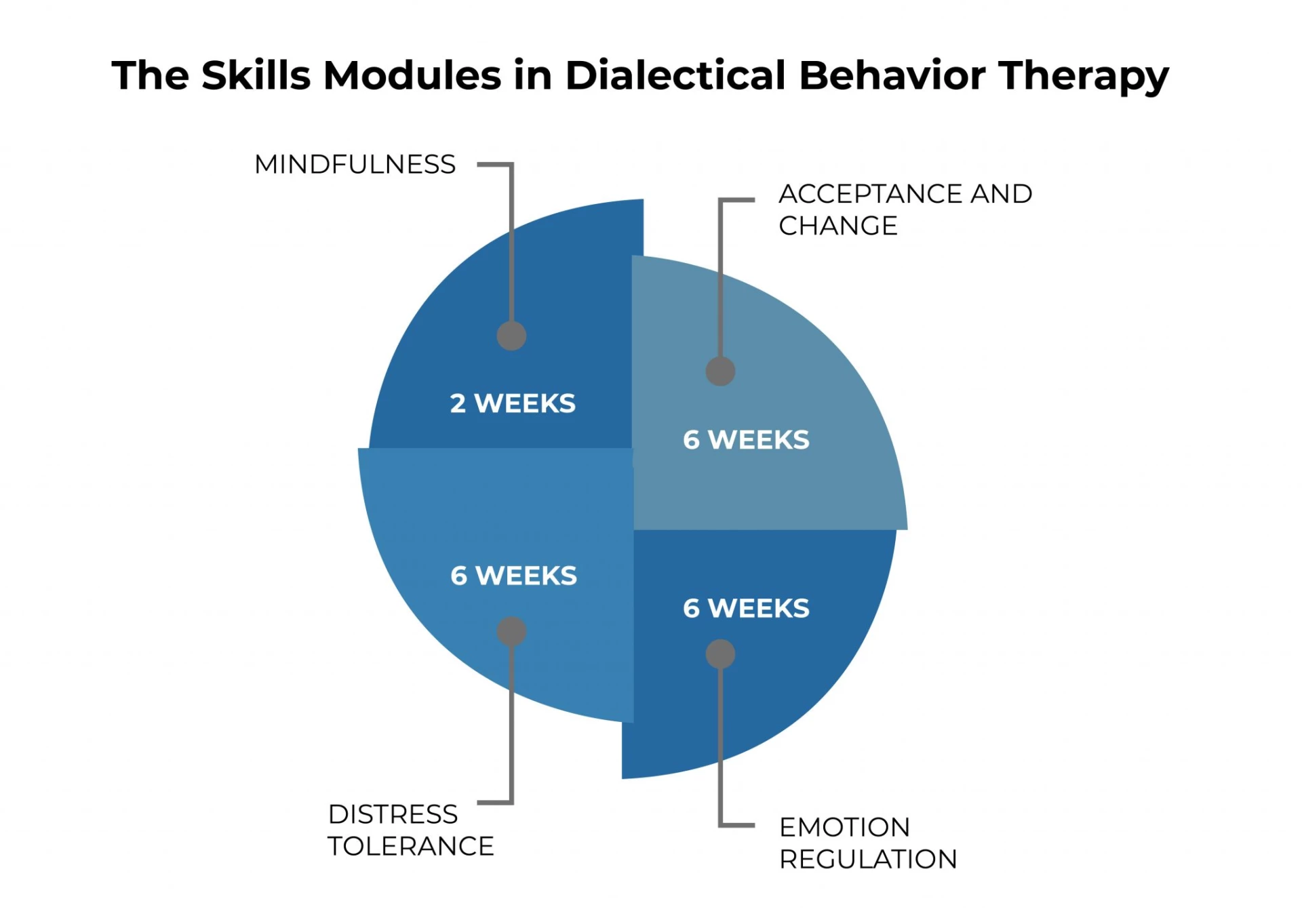
So these were the four modules of DBT. The weeks required to cover these modules are:
Mindfulness - 2 weeks
Acceptance and Change - 6 weeks
Distress Tolerance - 6 weeks
Emotion Regulation - 6 weeks
Chapter 4:
DBT v/s CBT
Dialectical Behavior Therapy and Cognitive Behavior Therapy are two terms that are often intermingled with each other. This chapter is all about CBT and DBT.
In this chapter, I will help you grasp how these terms are different from each other.


CBT v/s DBT
The two terms differ in many aspects. CBT is concerned with the interaction of your thoughts, feelings, and behaviors. While DBT tackles these concerns, it is primarily concerned with emotion regulation, mindfulness, and learning to accept discomfort. Look at these differences:
CBT v/s DBT for Treating Certain Illnesses:
Treatment does not always work for all mental diseases. An effective therapeutic strategy for depression and anxiety can increase eating disorders and personality problems.
CBT has been demonstrated to be extremely helpful in treating depression, and it is more likely than other types of therapy to bring depression into remission.
This type of therapy has also been shown to help with anxiety because it provides patients power over their rehabilitation. Obsessive-Compulsive Disorder (OCD), phobias, panic disorder, post-traumatic stress disorder, and sleeping problems have all been demonstrated to benefit from CBT.
DBT was developed to assist people who have been diagnosed with a borderline personality disorder. DBT focuses on helping people change their behavioral patterns rather than attempting to understand or speak through their problems. Patients who have developed patterns of extreme emotional reactions and impulsive behaviors in response to overwhelming sensations of sorrow and rejection can benefit from this sort of CBT.
When it comes to self-harm behaviors like cutting and prolonged suicidal ideation, DBT is often the most successful therapy. DBT strategies are also effective for sexual trauma sufferers.
Philosophies Used in CBT v/s DBT:
CBT is based on Stoic Philosophy and the Socratic Method, which emphasize thinking and logic. The Socratic Method employs critical thinking to challenge existing assumptions. This is beneficial for people who suffer from anxiety and depression because it allows them to perceive their difficulties in a more rational light.
Clients who are struggling with feelings of failure and inadequacy, for example, are encouraged to examine the facts. When have they actually succeeded in achieving a goal? Is there anyone else, friends, family, or coworkers who can attest to the client's success in various situations? Who or what are they utilizing as a yardstick for gauging success? Is that an accurate analogy?
DBT is primarily influenced by Buddhist and Zen mindfulness techniques. DBT instructs patients on how to utilize specific mindfulness practices to learn to live with pain in the world and accept things as they are rather than attempting to change them.
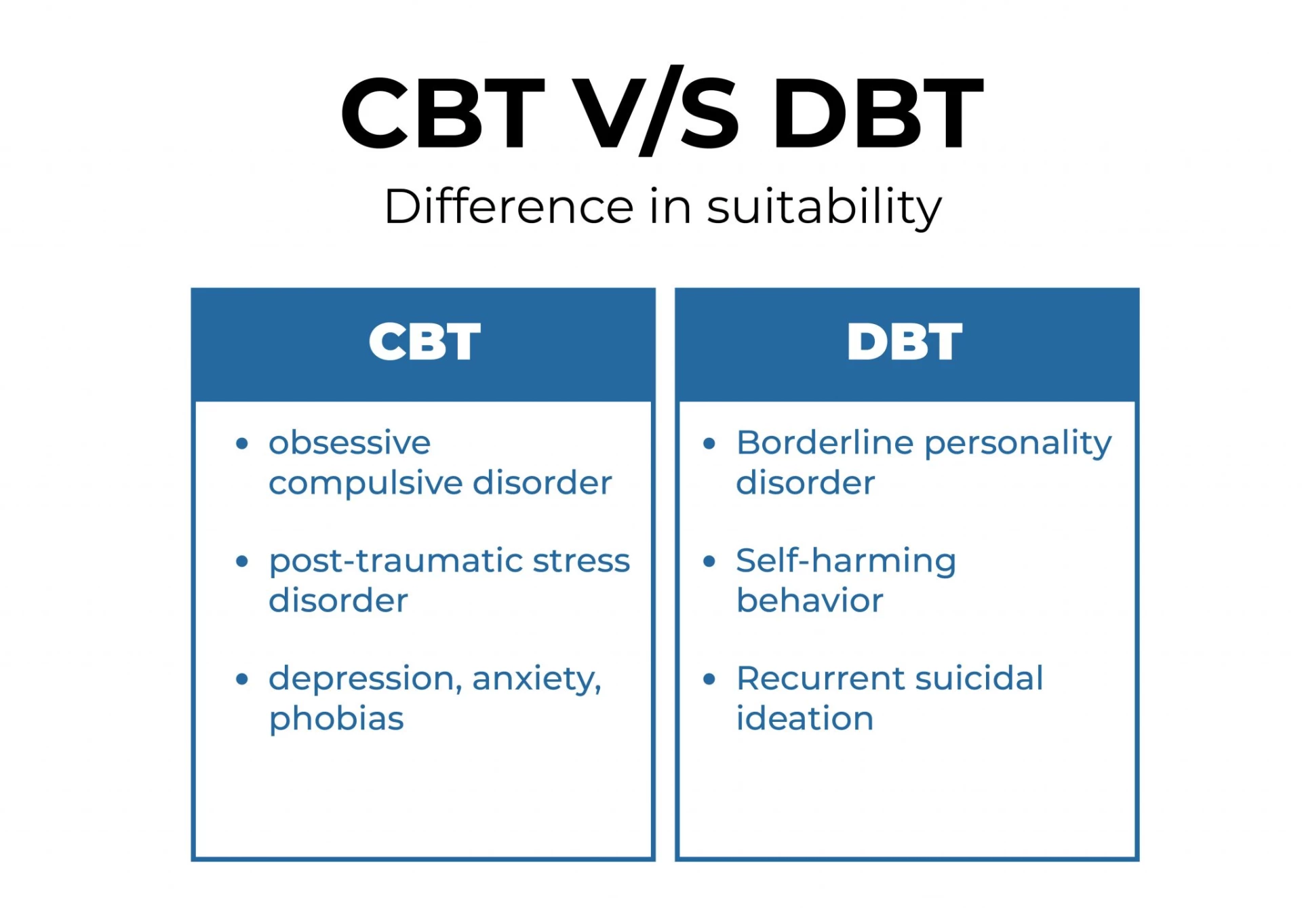
Difference in Suitability:
There is a difference in how effective each therapy is at alleviating the symptoms of mental illnesses. CBT has been demonstrated to be the most effective treatment for depression, anxiety, obsessive compulsive disorder (OCD), phobias, and post-traumatic stress disorder (PTSD) in studies.
DBT, on the other hand, is better suited to people who have BPD, self-harming behaviors, or recurrent suicidal ideation.
Difference in the kind of change created
CBT primarily assists clients in recognizing and changing harmful thought and behavior patterns in order to achieve a better and more realistic outlook on life.
Through validation, acceptance, and behavioral modifications, DBT primarily assists clients in regulating their intense emotions and improving interpersonal connections.
The Difference in Treatment Methods
CBT focuses on the interplay between your thoughts, feelings, and actions. While DBT addresses these issues, it focuses more on emotion regulation, mindfulness, and learning to accept discomfort.
CBT aims to teach patients how to detect when their thoughts are becoming problematic and how to redirect them. DBT teaches patients how to accept themselves, feel safe, and manage their emotions in order to control potentially harmful or destructive behaviors.
DBT therapy clients attend DBT skills training sessions, which are often taught in a group environment and consist of four modules.
Most patients also meet with a DBT therapist or coach once a week and receive DBT phone coaching when they need it the most. Patients who have mastered DBT skills for emotional regulation and social connection may be able to move on to more traditional CBT sessions to address specific negative thought patterns.
Difference in Time
CBT is usually finished in a short period of time. The sessions will concentrate on specific issues with specific goals in mind, so there will be something to strive towards.

Clients normally conclude CBT after they meet their goals which usually take 6 to 20 weeks. DBT, on the other hand, usually entails longer sessions where the therapist can explore the big picture and help the client work through multiple concerns. DBT typically takes at least 6 months to finish all of the courses, and in extreme cases, years.
How to tell if CBT or DBT is right for you?
There are several treatment models that can be utilized to treat someone who is suffering from a behavioral health problem.
Each style of therapy takes a different approach to the treatment process, and each has advantages and disadvantages depending on the person being treated. Two prevalent methods for treating mental health illnesses are cognitive behavioral therapy (CBT) and dialectical behavior therapy (DBT).
You'll notice that these models have very similar names, which helps to explain their relationship. DBT is a modified version of CBT, but its therapeutic strategy is sufficiently different from CBT that the two approaches are widely considered separate.
CBT and DBT are both supported by evidence of their efficacy, and they can be used to treat a wide range of mental health conditions. Several crucial considerations, however, may determine which model a therapist employs while treating a client.
So, in short, CBT has been demonstrated to be more beneficial than medication for depression, anxiety, OCD, phobias, and PTSD.
DBT is usually the superior option for borderline personality disorder, self-harm behaviors, and recurrent suicide ideation.
After looking at the differences between CBT and DBT, in Chapter 5 I'll tell you about the main advantages of DBT.
Chapter 5:
Core Benefits of DBT
This chapter will emphasize the benefits of DBT. Knowing the benefits of DBT will help you get a deep understanding and effectiveness of DBT in life.
DBT teaches patients how to accept themselves, feel safe, and manage their emotions in order to control potentially harmful or destructive behaviors.

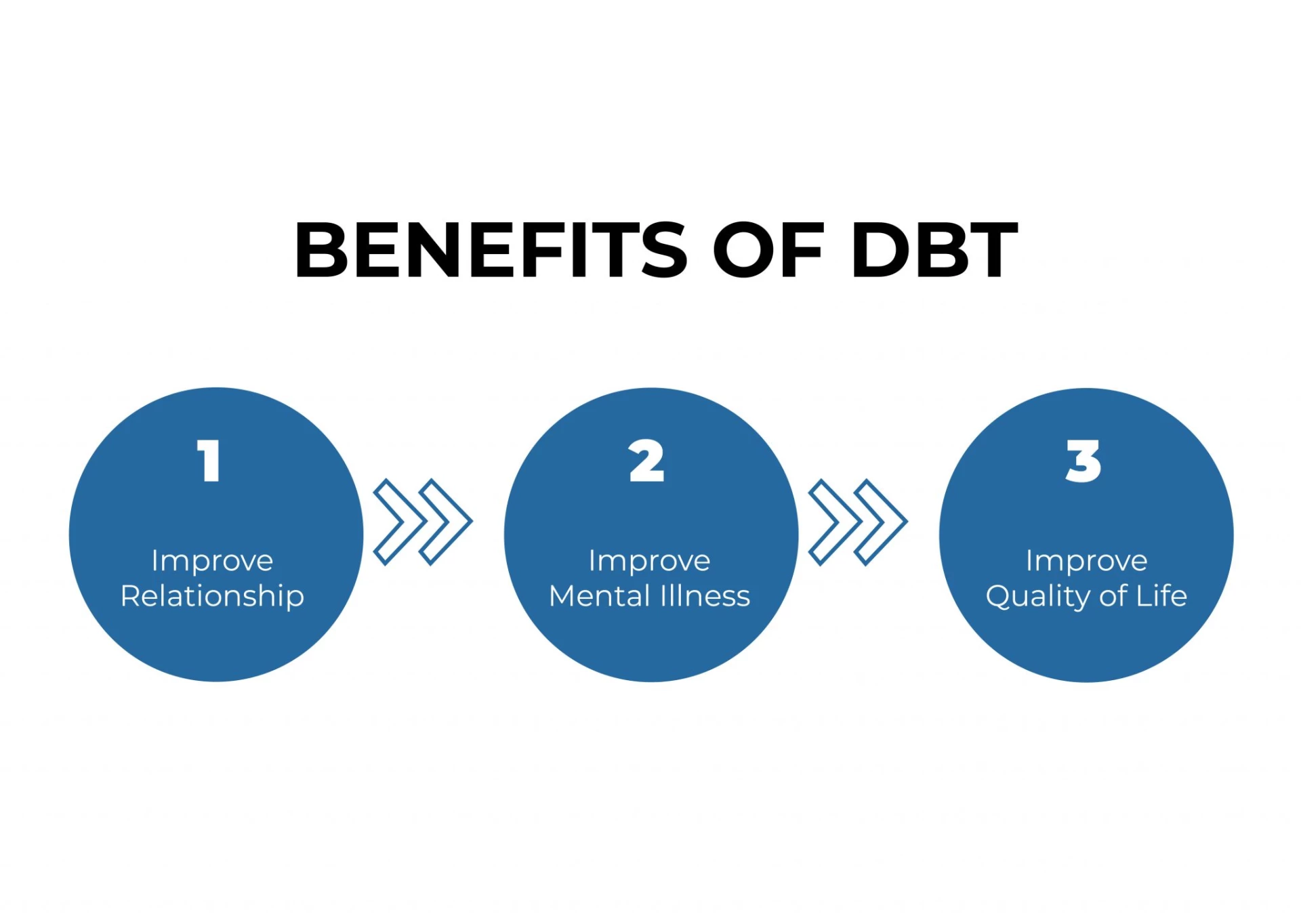
Benefits of DBT
A dialectical approach focuses on improving your ability to recognize and consider different points of view, challenge your assumptions, and strike a balance between changing your perspective and accepting things as they are in order to develop new perceptions and perspectives that will help you move forward and live a happier life.
Many of the persons in our therapy program have been diagnosed with borderline personality disorder and have attempted a variety of treatments to no avail. DBT has been shown to be successful in assisting people with a variety of issues, including:
- Emotions that are overwhelming
- Behavior that is impulsive
- Self-inflicted harm
- Suicidal ideation
- Use of substances
- Anorexia nervosa
- Trauma
- Relationships that are difficult and full of disagreement or arguments
Improve Your Relationship
When coping with mental health issues, having a strong support system is essential. Many types of therapy ignore this, expecting you to figure it out on your own.
However, DBT emphasizes the importance of our social ties in overcoming obstacles. Healthy relationships with respect boundaries and trust can benefit one's health and well-being in a variety of ways.
Improve Mental Illness
DBT's goal is to improve the symptoms of persons with mental illnesses, but it doesn't stop there.
The techniques taught by a DBT therapist can be used in a variety of situations. Mindfulness, for example, has been linked to a variety of other aspects of health and well-being in studies.
Once you've mastered this talent, you'll be able to use it in a variety of situations, including work, home, and play. Across the 12-month therapy and 12-month follow-up periods, DBT patients had lower rates of suicide attempts thoughts, psychiatric hospitalization, medical risk of para-suicidal behavior, angry behavior, and emergency room visits.
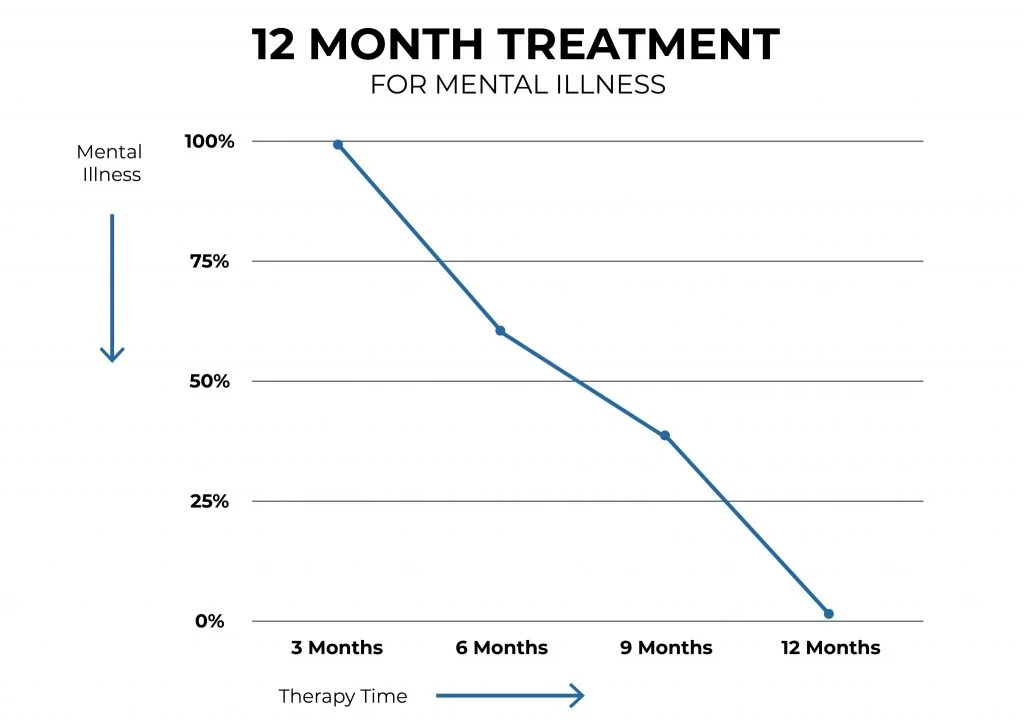
Improve Quality of Life
One of DBT's key goals is to improve one's quality of life. You can't always control what happens to you, and that's a harsh fact. Mental health issues will be a part of some people's lives for the rest of their lives, and accepting this truth is crucial to moving ahead.
DBT seeks to improve people's quality of life by gently guiding them toward positive changes while also reassuring them that it's okay to find things difficult. Quality of life can be seriously impaired for persons who are experiencing intense and disruptive emotions. The modules for distress tolerance and emotion control truly shine here.
DBT (Dialectical Behavior Therapy) is an evidence-based treatment with several benefits. If you can locate a skilled DBT therapist in your region and afford DBT treatment, you have a good chance of overcoming even your most severe symptoms and habits.
DBT-trained therapists have the ability to help you recover from addictions and psychiatric problems like Borderline Personality Disorder (BPD), as well as learn the skills you need to improve your quality of life.
Is DBT effective?
People can discover effective strategies to regulate and express strong emotions with this approach to therapy since it can help them improve their coping abilities. DBT is also beneficial independent of a person's age, gender, gender identity, sexual orientation, or race/ethnicity, according to researchers.
For BPD
DBT has been shown to be successful in the treatment of borderline personality disorder (BPD) and in lowering the risk of suicide in people with BPD in studies. More than 77% of persons with BPD no longer satisfied the diagnostic criteria for the disorder after a year of treatment.
For Suicidal Behavior
Most studies found that therapies that included skills training as a treatment component were more successful than enhanced usual care in reducing suicidal attempts and self-harming behaviors.
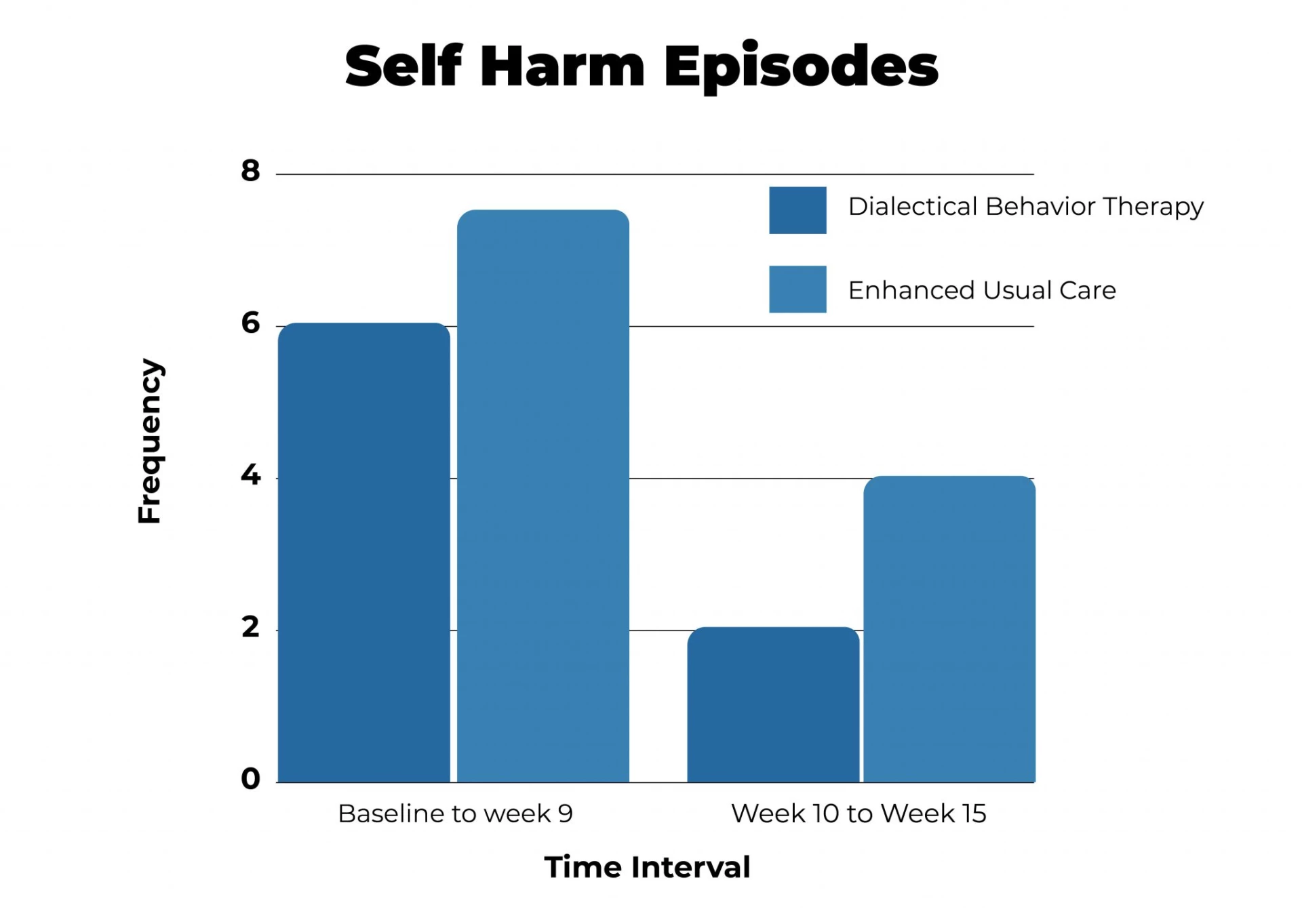
For Other Conditions
The majority of DBT research has focused on its effectiveness for people with borderline personality disorder who have suicidal and self-harming thoughts, although the therapy could also be effective for other mental health issues. This sort of therapy, for example, appears to be useful in the treatment of PTSD, depression, and anxiety.
DBT has been shown to be particularly successful in reducing self-harm, suicide attempts, and inpatient treatment days. It's also worth noting that DBT treatment resulted in a significant reduction in disorder-related direct and indirect monetary expenditures.
After learning about the benefits of DBT, I'll tell you about DBT steps that can help you enhance your self-esteem in the next chapter.
Chapter 6:
Steps in DBT that can boost your self-esteem
In this chapter, you will look at those steps that can help to boost self-esteem in DBT sessions. Self-esteem is made up of one's self-perceptions as well as emotional states including triumph, despair, pride, and humiliation and it is very important in Dialectical behavioral therapy because without this you cannot do a successful DBT session.
So, these are some steps from DBT which can boost your self-esteem.

Be Fair
Maintain a level of fairness in your interactions with people. Don't point the finger at them and don't assume full responsibility.
Also, be fair to yourself! Remember to congratulate yourself by telling yourself things like "I'm doing the right thing," "it's OK to look after myself," and "my needs are important too." Make a few cheerleading statements of your own.
They should connect with you and feel natural, but they should also be a little challenging. People who are treated fairly and given equal opportunities are better equipped to contribute to the community's social and economic growth and success.
No Excessive Apologies
Don't go overboard with your apologies. Make no apologies for requesting something or saying "no." Don't make an apology for something you didn't do or for which you have no remorse.
It's easy to try to "soften" the blow by apologizing to someone, but this doesn't assist them and makes you feel much worse.
Tell the Truth
Maintain honesty in all of your interactions, both with yourself and with others.
It may be tempting to tell a white lie or makeup justifications to avoid having to say something unpleasant, but this has a detrimental influence on your self-esteem. Simply speaking your truth is far more empowering.
You may be kind and honest at the same time. When my mother thinks back on difficult periods in her life, she constantly states that the word TRUTH and keeping true to herself brought her through.
Stick to your Values
Your self-esteem rises a little each time you make a decision that is in line with (or matches) your ideals. Every time you disregard your values, your self-esteem suffers a minor setback.
You improve your self-esteem over time by making decisions and doing things that align with your ideals. Don't shortchange yourself by selling yourself short on your values. But first, you must sit down and seriously consider your essential values.
After learning about DBT Steps that can help you raise your self-esteem, the next chapter will focus on Tips to Become a Successful DBT Therapist.
Chapter 7:
Tips to Become a Successful DBT Therapist
This chapter will concentrate on some useful tips for DBT therapists and some of the DPT techniques which can help to do sessions with the clients.

Dialectical Behavior Therapy Techniques
DBT has evolved into an evidence-based psychotherapy approach used to treat a wide range of conditions. DBT is frequently used in the following contexts:
Group Therapy
Patients are taught behavioral skills in a group setting during group therapy. The goal of group skills training is to improve the patient's capabilities by teaching them new skills that they can apply to other aspects of their lives.
Structured and psycho-educational group activities are included in group skills training. Individual therapy is supplemented by group sessions, which are usually held once a week and last between 2-2.5 hours.
Individual Therapy
Individual therapy with a trained professional in which a patient's acquired behavioral skills are applied to their specific life challenges. Individual therapy's goal is to increase motivation to address life-threatening behaviors, therapy-interfering behaviors, and quality-of-life-interfering behaviors.
Individual therapy consists of weekly standard DBT sessions that include dialectical and validation treatment strategies.
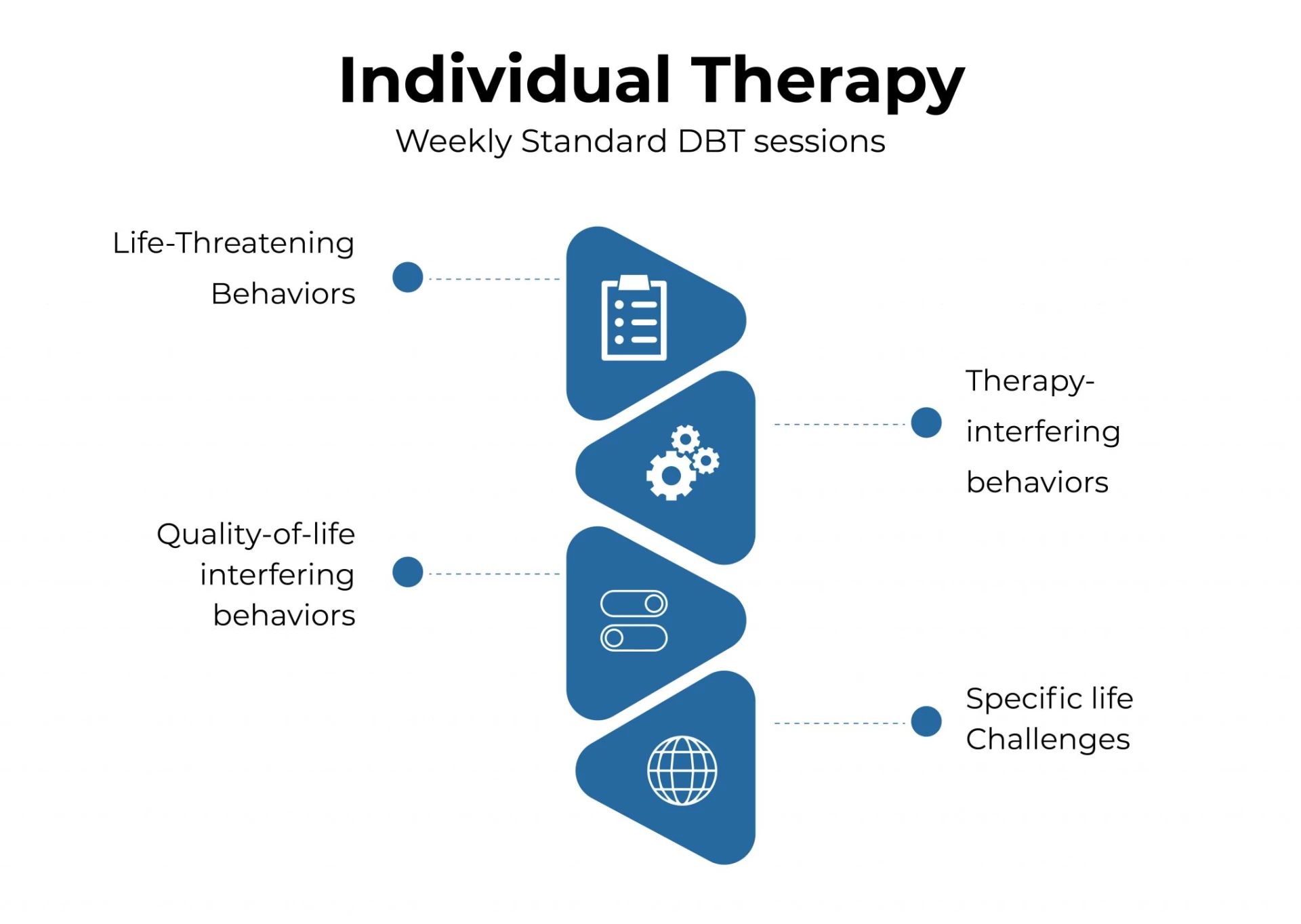
Phone Coaching
Patients can call the therapist between sessions to get advice on how to deal with a difficult situation they are currently in. DBT is the only psychotherapy model in which intersection contact is required for treatment. Intersession contact is intended to ensure skill generalization through coaching. Intersession contact consists of coaching calls that typically last between 10 and 20 minutes. The client does not need to be in crisis to contact the therapist, and the frequency should decrease as the client progresses through the program.
Consultation Team
The DBT therapist consultation team is intended to be therapy for the therapists as well as support for DBT providers working with people who frequently have severe, complex, and difficult-to-treat disorders.
The consultation team is intended to assist therapists in remaining motivated and competent in order to provide the best treatment possible. Teams of individual therapists and group leaders who share responsibility for each client's care typically meet weekly. Each member of our team has received extensive training.
DBT Skills
DBT regards the therapeutic alliance as the client's change-fostering mechanism, but it also recognizes that the client's support system outside of therapy is critical in assisting the client to address their issues.
DBT therapists frequently attempt to involve family members, friends, coworkers, peers in group therapy sessions, and others in the client's treatment. The following are general treatment objectives:
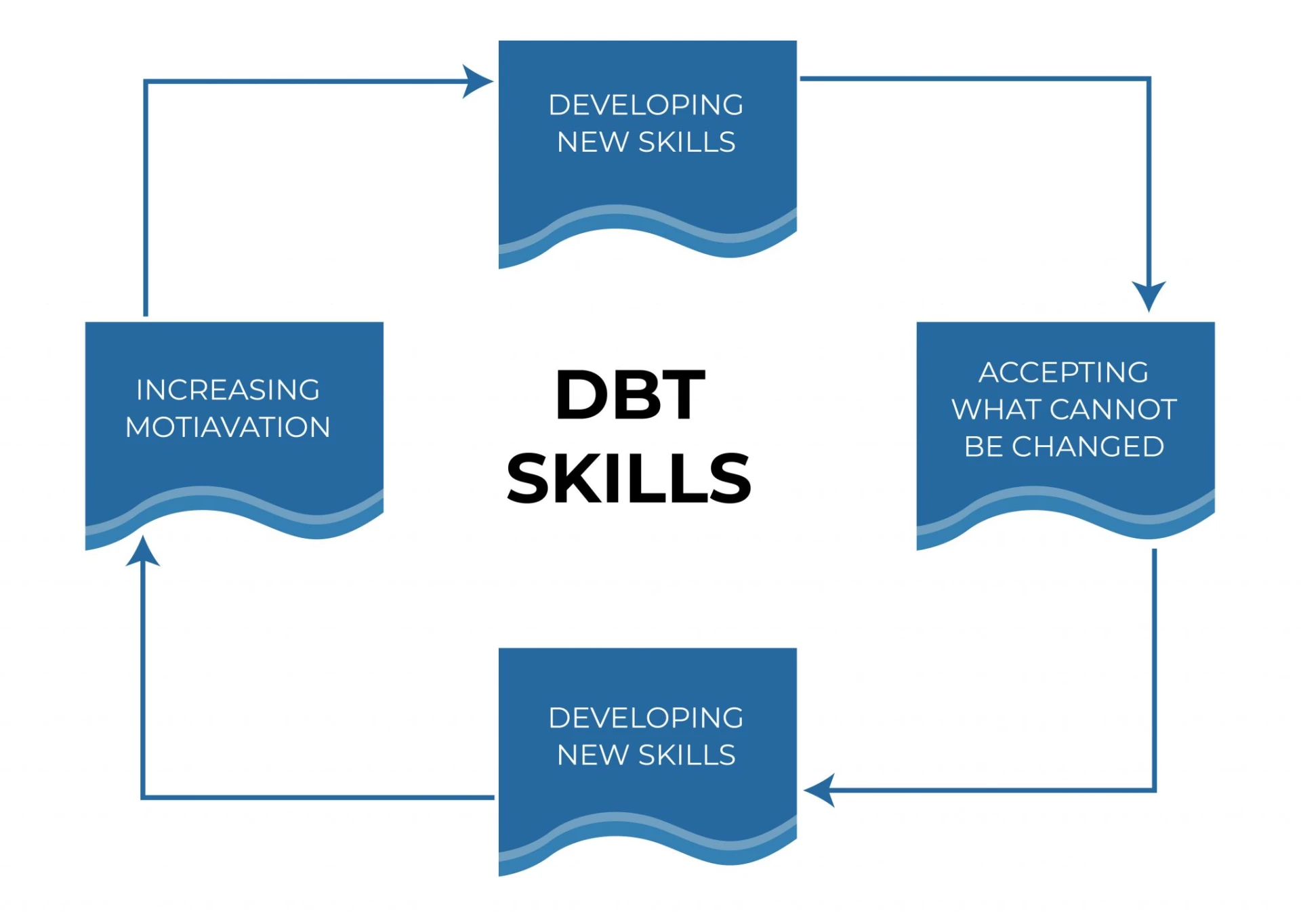
Developing New Skills
A key component of both individual and group therapy sessions is assisting clients in developing new strengths and skills so that they can successfully interact in the world.
Increasing Motivation
DBT uses therapeutic techniques and the involvement of family members and peers to keep the client's motivation high.
Accepting What Cannot Be Changed
Despite all of the potential therapeutic techniques available in DBT and the constant training and updating of the therapist's skills, there are always facts about life that are beyond our control.
Clients are frequently upset about things they cannot change. Helping clients accept and adjust to certain aspects of life is an important part of DBT.
Understanding the Client's Capacity for Change and Motivation to Change
DBT therapists are trained to understand and recognize the client's capacity for change and motivation to change.
Therapists are trained to work with clients at their level, assisting them in developing their motivation and capacity for change. Therapists ensure that the client's new skills learned in therapy can be applied in the real world.
Online Resources for DBT therapists
Here are some useful resources available for DBT. I have also listed few certifications that can help you to become a DBT therapist.

Online Apps to practice DBT skills
Individuals seeking Dialectical Behavior Therapy (DBT) have a particularly large gap between treatment need and treatment availability, and mobile apps based on DBT may be effective in expanding access to care and supplementing in-person DBT.
So These are the following apps listed below:
DBT Diary Card and Skills Coach App:
This is the only app on the market produced by a certified DBT practitioner. 3 Apps to Practice Your DBT Skills DBT psychologist, which essentially means you'll have a DBT professional with you at all times.
This full DBT app includes coaching to help you understand how and when to use the skills, a customized diary card that you can customize with the skills and targets you want to work on, progress charts and graphs, and a DBT reference section that lays down everything DBT.
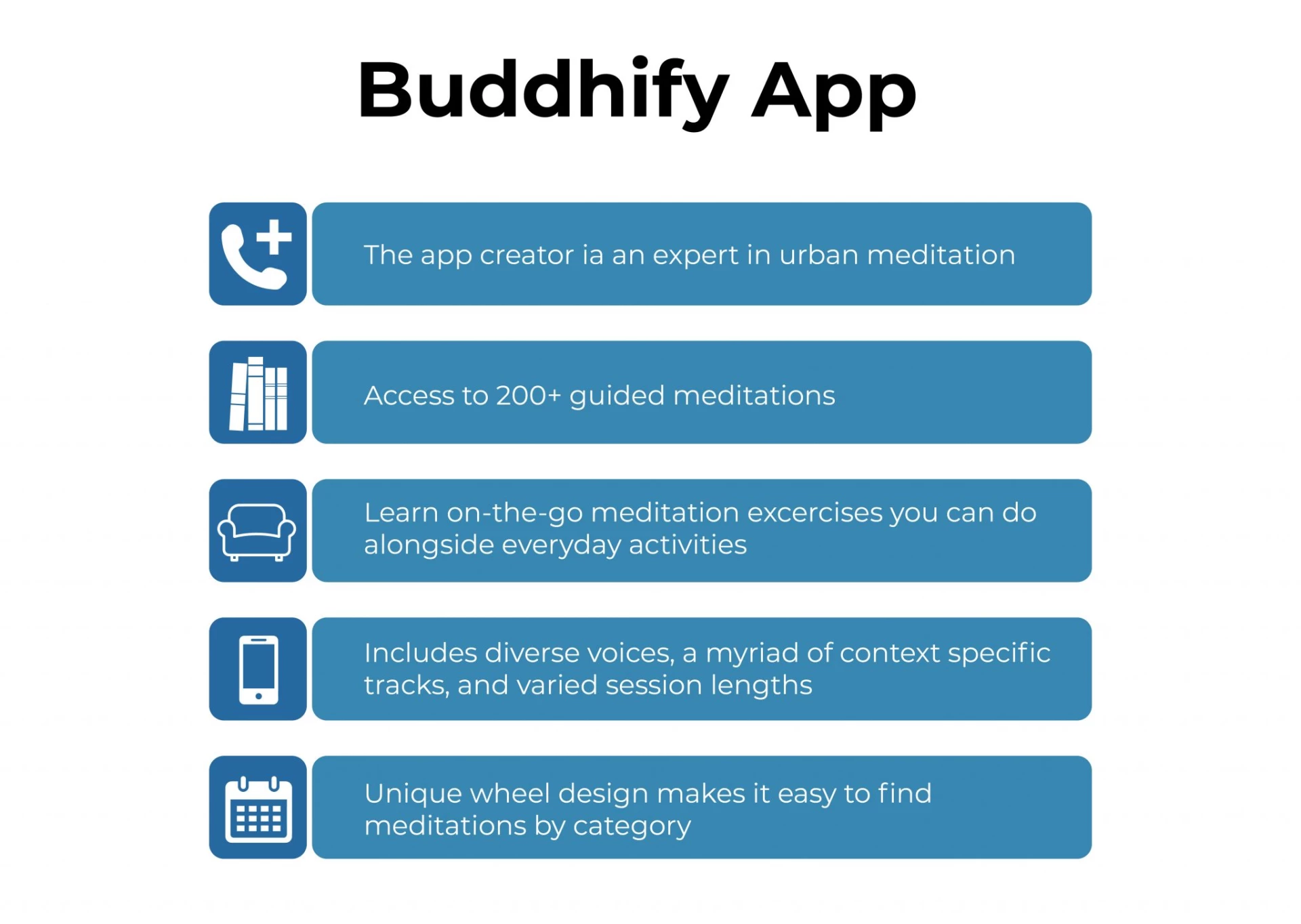
Buddhify App:
Mindfulness is at the heart of DBT. This app is fantastic since it allows me to access guided meditations according to my current mood or need.
"Modern mindfulness wherever you are," according to Buddhify. It stimulates you by asking "What are you doing?" and offers possibilities such as "walking in the city" or "difficult feelings."
It looks like the wheel from Wheel of Fortune. When you tap on what you desire, it offers more customized meditations based on time and preference. It also maintains track of your mindfulness practice on a chart, which encourages me to practice and be more consistent.
DBT trivia and Quiz App:
Anyone interested in DBT can take and learn from this simple quiz. This app will teach you new skills in a fun, engaging way, whether you're a novice or a seasoned DBT user. Anyone interested in DBT can take and learn from this simple quiz.
This app will teach you new skills in a fun, engaging way, whether you're a novice or a seasoned DBT user. Each level offers a set of questions centered on a specific topic. All you have to do is select the correct answer more often than not, and you'll be quickly advanced to the next level.
Each round you complete will provide an explanation for why the solution is the way it is.
Online Certification Available for DBT
Not all providers provide comprehensive DBT treatment while adhering to the research-based treatment protocol. DBT is a complex treatment modality that requires extensive training and ongoing feedback for providers. Clients and providers must participate in all four components of DBT, including individual DBT therapy, skills training, phone coaching, and consultation team.
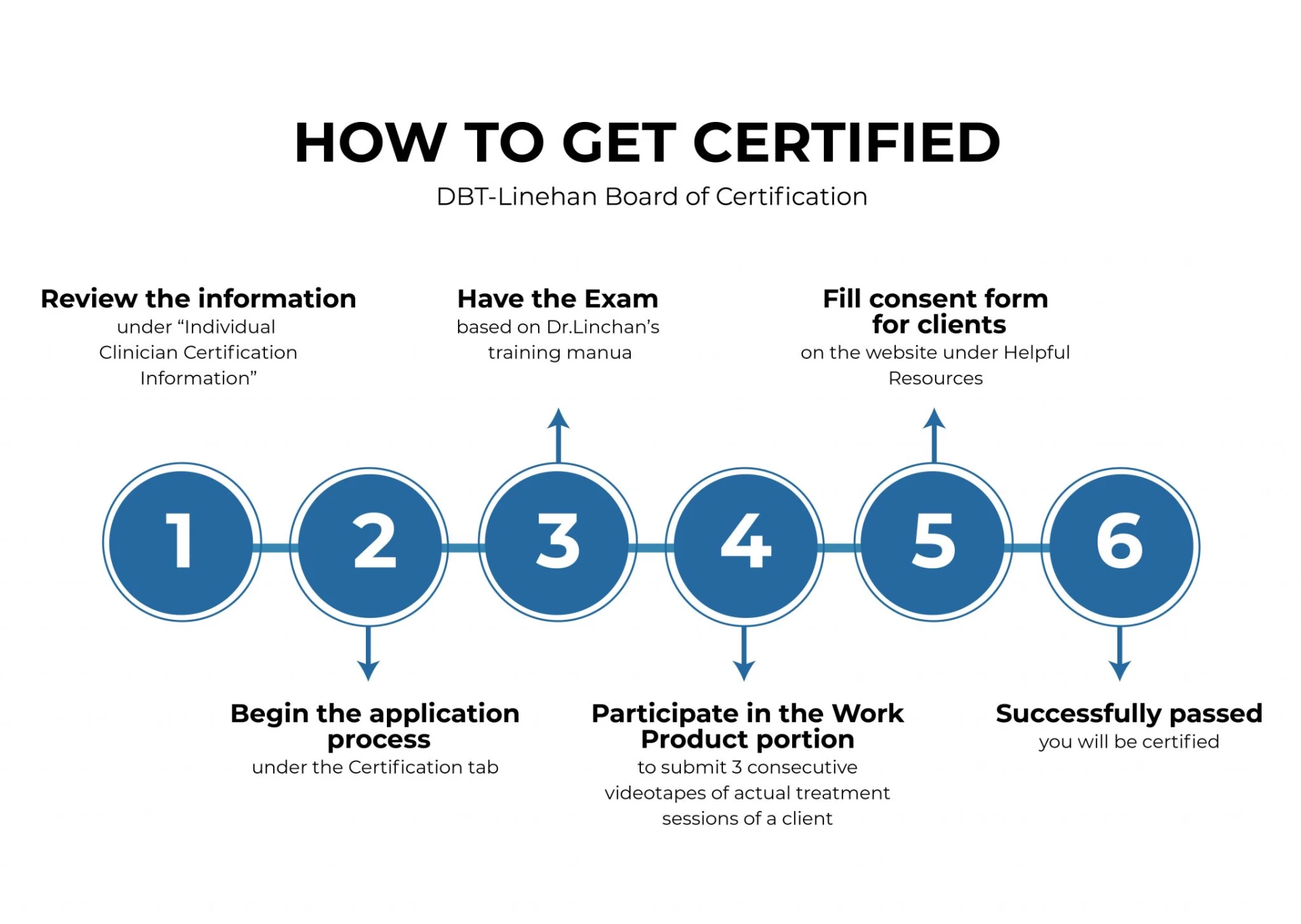
The DBT-Linehan Board of Certification is the certification body that assists people in clearly identifying individual DBT providers and treatment programs that have the knowledge and skills to deliver DBT in accordance with the treatment model developed and researched by Dr. Linehan and colleagues.
Finding DBT-Linehan certified clinicians or programs can be a good way to ensure that the provider is qualified and practices DBT on a regular basis.
DBT-Linehan Board of Certification-approved programs must have a DBT team leader who is a DBT-Linehan Board of Certification, Certified Clinician.
The program invites DBT treatment experts to observe, review, and evaluate their DBT program's practices. The lengthy process includes scoring responses to a Program Fidelity Scale questionnaire as well as reviewing program documents and files to determine the structure of the DBT program.
The site reviewers are treatment experts who conduct interviews with treatment providers and clients as well as on-site observations of DBT program practices in action.
Receiving DBT-Linehan Certification is a significant achievement for any DBT provider. This is the only DBT certifying body with the active participation and endorsement of Marsha M. Linehan, Ph.D., the DBT's founder and developer.
The program has been thoroughly reviewed and examined to ensure that the clinicians and programs are qualified and intend to provide gold standard care. It assures patients and their families that the facility has sufficient knowledge of assisting patients with severe emotional and behavioral problems.
So, while engaging in any certification program or online course, must make sure that the offering platform is DBT-Linehan certified. The courses which we recommend to join include Psychotherapy academy, Udemy, APT, Laurier, behavioral tech, class central, etc.
Conclusion
Congratulations!
You've completed this guidebook admirably, and you now have all the information you require regarding Dielectric Behavior Therapy. I hope that this article will help you in your practical life and will give you a deep beneficial understanding of DPT.
Implement all of the actions outlined in this guide for your therapy.
What section of this guide was most informative to you?
Which DBT benefit drew your admiration the most?
Which disorder do you want DBT to help you with?
Have all of your questions been answered in the guide? If you still have queries about any area, let me know in the comments section below.
Frequently Asked Questions
What conditions can DBT help treat?
How long does it take for DBT to start showing results?
Who is DBT not recommended for?
Is DBT covered by insurance?
Now, let me walk you through some useful online resources that will help you.

